|
Hyperhidrosis USA - Micro ETS | Call 210-490-7464 Email info@dhnmd.com | The Offices of David H. Nielson, MD |

 |
 |
 |
| ETS Brochure | ETS Folleto |
| English | Espanol |
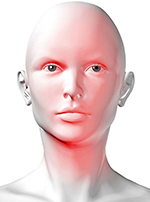
Facial Blushing - Hyperpyrexia, Red Burning Face Symptoms and Treatment
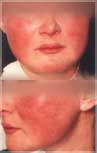
Facial blushing is often mis-diagnosed as Rosacea A red face is a typical manifestation of this condition. Fear of social situations can bring on blushing and is known as erythrophobia and erythromelalgia. Blushing commonly originates at the upper chest or base of the neck and extends up to the forehead, ears and can even spread down to include the trunk and legs. Facial sweat often accompanies blushing and feelings of burning or tingling.
Hyperpyrexia (feelings of burning, heat or tingling) is commonly associated with blushing episodes several times a day, and is actually much more debilitating to the individual than the mere appearance of blus on the skin. This condition of hyperpyrexia associated with facial blushing is little understood and not typically recognized by many physicians. Functional impairment arises from the intense "burning" sensation that becomes so uncomfortable that the individual has to actually stop what they are doing because of the severe inability to concentrate or follow through with the task at hand. Many patients have described the feeling they experience from hyperpyrexia as "hot flash or burning." This sensation envelops their face/head/neck to such an extent that they seek seclusion to "cool off".
A 19 y/o man shares the story of his difficult journey: "The burning in my eyes and face is finally gone → following Micro ETS. I looked into facial blushing causes and treatments, I looked into EYE Pain in social interactions and searched Micro ETS in Texas. Wow, after Micro ETS, I don't feel the heat and burning in my cheeks and eyes, especially in social interactions any more. I even drove in a car with the windows down, wind in my face and no blushing or burning, for the first time in so many years." A 32 y/o female from Kansas City, KS shared this: “I woke up this morning without the burning in my face for the first time in such a long time. I don’t feel any stress at all right now with the burning gone from my face.” Micro ETS caused immediate improvement in her blushing/burning, the moment the nerve was precisely divided where it crosses the 2nd rib head, just above the T2 ganglion without disturbing any tissue at all to find the nerve. No drooping of the upper eyelid ever occurs since the nerve doesn’t have to be dissected from the inner chest wall tissue to find it. “Prior to Micro ETS, Emotional triggers would cause many episodes each day x 20 years of burning starting in her cheeks then spreading to her entire face and upper neck along with redness (blush).” She relates: "beta blockers didn’t improve the blushing/burning at all, completely ineffective.” She would only work from home due to the severe burning (facial Hyperpyrexia) and blushing of her face and upper neck when around others. Now, with HUGE improvement in her face/neck not feeling the frequent burning anymore, she feels much more self-assured and confident in being with others and now feels comfortable working with others outside of her home, since the blushing/burning has improved. She can “BE HERSELF" around others. Medications are seldom helpful for this intense "hot or burning" feeling. Beta blockers (i.e.: commonly used but little help).
| ||||||||||||||||||||||||
Effective treatment for facial blushing
with hyperpyrexia is Micro ETS of T2.Precise
division of the sympathetic nerve exactly where it crosses the
upper edge of the second rib and any kuntz nerve Persistent facial blushing after sympathectomy can occur if any kuntz nerve that crosses the second thoracic rib is left intact, and can therefore continue to carry nerve signals to the face. In the many redo's Dr. Nielson has performed for persistent facial blushing, he has found that the most common reason for persistent blushing has been missed Kuntz nerves crossing the second thoracic rib. He has also found, less commonly, the sympathetic nerve had been divided at the T3 level by mistake rather than the T2 level. T2 Sympathetic Innervation
to The Sweat Glands of the Face Over several years of experience in treating patients with recurrent and/or persistent sweating of the face after undergoing T2 sympathectomy,Dr. Nielson has found that persistence of any sympathetic nerve innervation across the second rib level, just above the T2 ganglion, plays a significant role in persistent sweating conditions of the face after undergoing a T2. T3, or T4 sympathectomy. It is apparent in some patients that there are neuronal contributions from lower levels such as the T3 that pass up over the second rib level on their way to the face that participate in the sweating symptoms of the face. Some physicians misunderstand the sympathetic nerve innervation of the face and believe in order to successfully treat facial sweating it is important to cut the sympathetic nerve at the T1 level or above, thereby causing the dreaded Horner’s Syndrome. In Dr. Nielson's experience, he has found this not to be the case. In summary, for successful treatment of facial sweating, it is imperative that all sympathetic nerve innervation crossing the second rib level be divided as opposed to clamped or having lower levels cut or clamped. Also, accessory nerve branch pathways bypassing the T2 ganglion can or may contribute to persistent facial symptoms.
Please contact us for more information on hyperhidrosis: Call 210-490-7464 Email info@dhnmd.com or Submit a questionnaire.
|
||||||||||||||||||||||||
| HOME | CONTACT US | TERMS OF USE | NOTICE OF PRIVACY PRACTICES | SITEMAP | Call 210-490-7464 Email info@dhnmd.com | ||||||||||||||||||||||||
| MICRO
ETS | HYPERHIDROSIS | FACIAL
BLUSHING | RAYNAUD'S | FAQs | TESTIMONIALS | SIDE
EFFECTS | VIDEO | DR
NIELSON | CONTACT US FACIAL SWEATING | SWEATY HANDS | SWEATY FEET | ARMPIT SWEATING | | ALTERNATIVE TREATMENT | IN THE NEWS RESULTS MAY VARY FROM PERSON TO PERSON. Copyright © 2021 Hyperhidrosis USA. All rights reserved. |
||||||||||||||||||||||||